
Category: Auto Immune Disease


Is Giving UP Gluten REALLY Necessary for Hashimoto’s Patients, or Just Fad Hype?
Unless you are newly diagnosed, chances are you have heard a lot about the connection between eating gluten (a protein found in wheat, barley, rye, oats) and auto immune diseases like Hashimoto’s.
You also have probably heard from your doctor, online nutritionists, and many mainstream media outlets and late night talk show hosts saying it is a lot of BS, and that you actually NEED gluten to be healthy.
So Who Is Right?
And also, just how strict do I really need to be? Can’t I have a little cheat? What if I don’t have any gut symptoms?
To find out the answer, I searched through research articles on PubMed. I already knew my stance on the issue, but wanted to make sure there was current research that supported it.
The September 2015 edition of the journal Gastroenterology found high “proportions of patients with NCWS or CD develop autoimmune disorders, are ANA positive, and showed DQ2/DQ8 haplotypes”. (note- NCWS is non-Celiac wheat sensitivity.)
In the March 2015 journal Cerebellum, gluten was further linked to neurological disorders such as gluten ataxia, where there were no gut symptoms whatsoever, and occurred most commonly in patients with Hashimoto’s and other auto immune diseases. Check out this quote from the study:
“As with celiac disease, patients with GA (gluten ataxia) are often found to have an increased prevalence of additional autoimmune diseases the commonest of which include hypothyroidism, type 1 diabetes mellitus and pernicious anemia. Gastrointestinal symptoms are seldom prominent and are not a reliable indicator for the presence or absence of enteropathy. In this respect, gluten ataxia resembles dermatitis herpetiformis, an autoimmune dermatopathy triggered by gluten where gastrointestinal symptoms are not prominent even in the presence of an enteropathy.” (parenthesis and bold added by me for emphasis and clarification)
Wow. That is pretty powerful. How many of you with brain symptoms has ever had your doctor consider a possible gluten connection?
Did you know that a study from 3 years ago showed an increased need for T4 in patients with atypical Celiac disease?
How about that the need for increased T4 dosage reversed when the patient adopted a gluten free diet?
This study was in the March 2012 journal of Clinical Endocrinology and Metabolism. Have you ever had your endocrinologist consider that this may be another reason your T4 is not working as it should, or did they ridicule you when you asked about it?
As far back as 1999, the Italian Journal of Gastroenterology and Hepatology concluded the following:
“The prevalence of coeliac disease in patients with autoimmune thyroid diseases is significantly increased when compared with the general population (p = 0.009) but not with patients affected by non autoimmune thyroid disorders (p = 0.18). We suggest a serological screening for coeliac disease in all patients with autoimmune thyroid disease measuring anti-endomysial antibodies, considering that early detection and treatment of coeliac disease are effective in preventing its complications.”
I could go on and on with studies that show the connection between gluten reactions, both non-celiac and celiac, and auto immune diseases, but it would quickly turn into a book.
The 2013 study in the journal Brain and Nerve by Yoneda even showed connections between Hashimoto’s encephalitis and gluten ataxia, which caused not only thyroid symptoms but neurological symptoms. Thus gluten intake actually triggered not only reactions in the thyroid but also the brain.
Ok, so there IS a connection, but can’t I have an occasional cheat?
I remember talking to my friend Dr Datis Kharrazian about this. My wife had gotten seriously ill from her thyroid and mine was wreaking havoc on my life as well.
He asked if we were gluten free. I told him “mostly, like 95%.”
His response was that there was no such thing as mostly gluten free…just like you could not be mostly pregnant…you either ARE or ARE NOT…
It wasn’t what I wanted to hear, but it was what I needed to hear. He then told me something that the immunologists at Cyrex Labs confirmed when I had a consultation with one of their top doctors.
Just ONE exposure to gluten, one little bite of a “cheat”, could trigger an immune flare up that lasts 6 months to one year.
One year…that is HUGE.
I highly recommend that you go onto www.PubMed.org and search for yourself. The number of research studies is mind boggling.
Also check out www.CyrexLabs.com to read about the cutting edge tests that they are running for food reactions, environmental toxins, chemicals, metals, etc.
I hope this gives you some helpful info, and be sure to talk this over with your functional medicine or functional neurology practitioner for customized help.
You can follow me @drkirkgair or www.Facebook.com/ThyroidInfo
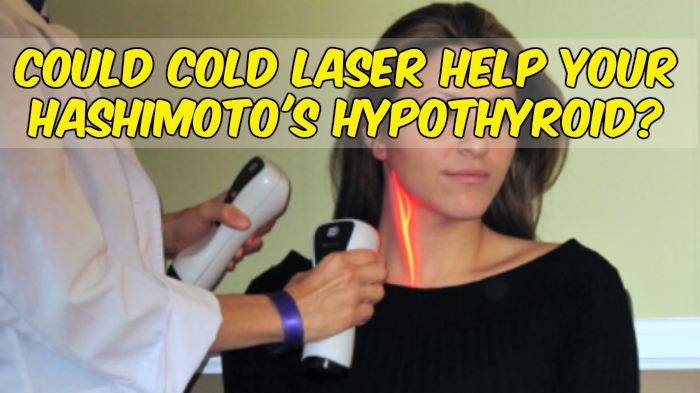
Could Cold Laser Be The Next Big Thing In Helping Thyroid Patients?
A lot has been written about the connections between Hashimoto’s and gluten, environmental toxins, leaky gut, etc. However, very little has been discussed about the potential use for Cold Laser therapy, even though several recent research studies found some promising results.
Hashimoto’s antibodies can lead to destruction of thyroid tissue, which can result not only in the symptoms of thyroid dysfunction, but also changes in thyroid appearance on ultrasound, and the presence of abnormal blood markers.
Currently, most traditional medical treatments aim to control the symptoms or get the TSH and T4 into the medical normal range while often ignoring the underlying root causes and the destruction that occurs in the gland.
The exciting thing about these studies on lasers and their effects on the thyroid is that they appear to not only trigger tissue regeneration, they also seem to help normalize function and decrease the need for medications, without any side effects.
The most recent study comes out of the July 2015 edition of the journal Photochemistry and Photobiology. In this study, the thyroid glands of rats were damaged with gamma radiation, and then were treated with low level laser of 632 nanometers for 6 sessions. The study concluded that the laser improved the rats thyroid function, liver function, antioxidant levels, and blood cell markers. No side effects were noted. http://www.ncbi.nlm.nih.gov/pubmed/25975382
The August 2014 edition of the journal Photomedicine and Laser Surgery found that cold laser treatment to patients with autoimmune thyroid disease significantly increased levels of transforming growth factor-β1 (TGF-β1). (www.ncbi.nlm.nih.gov/pubmed/25101534) Why is this important? The August 1991 edition of the Journal of Autoimmunity found that TGF-β1 could calm down and suppress auto immune attacks, and that it may even prove helpful in causing remission of Graves disease. (http://www.ncbi.nlm.nih.gov/pubmed/1777015)
Patients with autoimmune thyroid disease often have altered blood flow within the thyroid. The 2012 journal ISRN Endocrinology found that 10 laser treatments improved blood flow within the thyroid, as visualized with Dopplar ultrasound. (http://www.ncbi.nlm.nih.gov/pubmed/23316383)
But perhaps the most exciting study I came across was in the August 2010 journal Lasers in Surgery and Medicine. Patients were given 10 treatments over 5 weeks. They found that all patients needed less thyroid medication, including 47% who did not require any medication through the 9-month follow-up. Can you imagine being able to go 9 months without needing thyroid medication?
Furthermore, the medication dosage needed in the other participants decreased, and remained decreased even 9 months later. TPOAb (thyroid antibody) levels also decreased, and thyroid tissue appearance improved on ultrasound. This means that thyroid tissue damaged by auto immune attacks was actually getting repaired with laser stimulation. Again, no side effects were noted. (http://www.ncbi.nlm.nih.gov/pubmed/20662037)
These are just a few of the exciting studies that support the use of lasers in thyroid disease, but the applications go even beyond just the thyroid. As far back as December 1993, there was a far reaching study from Japan in the Keio Journal of Medicine that found that laser therapy on cancer cells “inhibits growth and increases cell-specific destruction”, and that “other immune system-related diseases, such as atopic dermatitis, some forms of eczema, asthma and asthma-related ulceration, have responded well to” laser therapy. I found numerous other studies that also suggested that cold laser was effective even for helping with thyroid cancers. (http://www.ncbi.nlm.nih.gov/pubmed/8126975)
So let’s review what these studies found. Cold laser therapy was shown to:
- Reduce TPO antibody levels
- Reduce the need for T4 medications in a majority of patients, even 9 months after treatment, and eliminate the need in nearly half the patients in one study
- Increase the amount of cellular antioxidants such as glutathione
- Improve thyroid tissue and vascularization on ultrasound examination
- Increase levels of transforming growth factor-β1 (TGF-β1), which calms down the auto immune activity and may have the potential to cause remission of Graves’ disease
- Decrease the activity of inflammatory molecules such as nuclear factor kappa beta and interleukin 6
- Stimulate the repair of tissue damaged by the thyroid auto immune attack
- Have no side effects
These are all pretty powerful findings. I was surprised to find the data going back over 20 years supporting cold laser’s use on auto immune diseases, considering that most of us have never heard about it in mainstream media or from our doctors.
Obviously more studies are needed, but the current research suggests that lasers may provide significant help for the growing numbers of auto immune thyroid patients out there. Have any of you out there tried this therapy or heard about it from your doctor? If you have, please comment with what your results have been.
Please check out my facebook page at www.Facebook.com/ThyroidInfo, or follow me on twitter @drkirkgair.
This information is for informational purposes only and should not replace the diagnosis and treatment of your qualified healthcare professional. Do not undertake using a laser on yourself without proper evaluation and supervision of a licensed healthcare provider. As always, Dr Gair recommends that you seek the help of a healthcare professional trained in functional medicine and following their advice.

Could Vitamin D Actually PREVENT Hashimoto’s, Diabetes, and Even Cancer? And If So, How Much Do You Need?
Ah, Vitamin D…the “sunshine vitamin”. When most of us hear about it, we usually just associate it with healthy bones…but it is actually so much more than that.
Many people have the mistaken idea that “all you have to do is get a little sun and you will have enough.” This simply is not the case, as I routinely find severe deficiencies even in kids and people who are outside all day playing sports or working.
Deficiency in the US is currently 41.6% of causcasians, 69.2% of Hispanics, and a whopping 82.1% of African Americans, according to a study in the Jan 2011 edition of the journal Nutrition Research. http://www.ncbi.nlm.nih.gov/pubmed/21310306
I got curious to see if there was any research that showed not just that vitamin D was good for those who already have auto immune diseases like Hashimoto’s and Diabetes, but if any studies showed it could help prevent your kids from developing the same disease. What I discovered in the research studies is very promising!
So what else does Vitamin D do besides make healthy bones?
It is involved with the regulation of over 900 genes, influences and modulates the immune system, modulates inflammation, has a role in fighting preventing cancer, and even plays a role in brain function and diseases like dementia and Alzheimer’s.
Vitamin D deficiencies are also associated with other conditions besides just Rickets and Osteoporosis, such as PCOS, Lupus, Diabetes, Celiac, and inflammatory bowel diseases.
Grain Brain author, Dr David Perlmutter, thinks optimal vitamin D levels are so important that has made a video that explains why he tests ALL his patients… http://www.drperlmutter.com/delightful-vitamin-d/
What Does The Research Say About The Link Between Low Levels and Auto Immune Disease?
When searching through peer reviewed articles on this topic, I found several promising studies.
In the May 2013 edition of the journal Endocrine Practice, they found the following:
“We demonstrated that serum 25OHD (vitamin D3) levels of HT (Hashimoto’s Thyroiditis) patients were significantly lower than controls, and 25OHD deficiency severity correlated with duration of HT, thyroid volume, and antibody levels. These findings may suggest a potential role of 25OHD in development of HT and/or its progression to hypothyroidism.” http://www.ncbi.nlm.nih.gov/pubmed/23337162
Several other studies found the same thing. One study in the 2015 edition of Scientific World Journal found that “lower serum D levels were associated with higher thyroid antibody levels.” http://www.ncbi.nlm.nih.gov/pubmed/25654127
Other studies also linked low vitamin D to Childhood Obesity, Inflammatory Bowel Diseases, Cancer, Diabetes, Insulin Sensitivity problems, and more.
Can Optimal Levels Reduce Risk?
In the May 2014 Journal of Endocrinological Investigation found that higher levels of Vitamin D on blood tests could actually reduce the risk of Hashimoto’s.
“Our study suggested that higher serum 25OHD levels was associated with decreased risk of HT (Hashimoto’s Thyroiditis) so that each 5 ng/ml increase in the serum 25OHD levels results in 19 % decrease in odds of HT.” http://www.ncbi.nlm.nih.gov/pubmed/24639121
This is huge. So if you raised your D level from a mild deficiency of 25 ng/ml to the recommended 50 ng/ml, you would decrease your odds by 115%. Pretty powerful for such an inexpensive supplement.
And the Dec 2012 journal AutoImmune Review found “Basic, genetic, and epidemiological studies indicate a potential role of vitamin D in the prevention of autoimmune diseases.” http://www.ncbi.nlm.nih.gov/pubmed/22776787
There were many more articles that had similar conclusions for not just Hashimoto’s but also other auto immune diseases ranging from Diabetes to Lupus to Rheumatoid Arthritis.
And this study from the British Journal of Dermatology in Aug 2002 even showed a protective benefit from cancer, as vitamin D was shown to help with the “inhibition of tumour invasion and metastasis potential” and that it has “an inhibitory effect on the spread of MM (malignant melanoma) cells.” http://www.ncbi.nlm.nih.gov/pubmed/12174089
So What Level Is Optimal, and How Much Is Safe And Necessary to Take to Get There?
When looking at all these studies, in general the minimum level seemed to be 50 ng/ml. Compare that to the fact that most patients are being told their levels are “fine” if they are in the 30 ng/ml range.
Other studies suggested that the target range should be 60-80 ng/ml for auto immune and cardiac patients, and between 80-100 ng/ml for cancer patients.
The Feb 2001 edition of the American Journal of Clinical Nutrition found that doses of 4000 IU (100 mcg) per day were safe. The Mayo Clinic has various ranges depending on the condition, and some doses are much higher than those in this study.
My recommendation is to find a good functional medicine practitioner and get your D3 level tested instead of just going off a chart for a condition. This way you and your provider can work at getting the right dosage for you to get into your optimal range.
When I have patients who are deficient in my office, we will usually start them off with a daily dose of sublingual D3 with cofactors and will test them each 1 to 2 months until we hit the target range.
Some patients may need only 4000 to 6000 IU per day, while others need it much higher. This is why blood testing is crucial, especially follow up testing. I have seen patients come in who had been on supplements for years who were still deficient.
So What Do I Do If I Am One Of Those Patients Who Remains Deficient Despite Supplementing?
First thing I would do is to look at which type of vitamin D you are taking. D2 has been shown to be ineffective at raising blood levels, yet that is the form I regularly see doctors prescribing. In fact, large HMOs still do this despite the evidence that it is ineffective. Studies show D3 to be more effective.
Second, if you have gut issues, such as Celiac disease, gluten sensitivity, Crohn’s disease, ulcerative colitis, or had gastric bypass surgery, it will be more difficult for you to absorb D3. This is why I utilize the sublingual forms with my patients. You may also require a form that has co-factors in it such as vitamin K for better utilization. Still others may have genetic issues that affect absorption.
Third, work with your doctor on gradually increasing your dose safely until you can get the level to increase. Once you get to your target level, then you will work on your daily level to maintain it at optimal. I would recommend testing the level at least twice per year.
I hope you found this article helpful. You can follow me at www.Facebook.com/ThyroidInfo, www.Facebook.com/LaserChiropractic, or @drkirkgair. You can also join my mailing list to get my latest blog posts sent to you free.
And remember to discuss all these issues with your healthcare provider before starting a supplementation protocol.